Home » Blog
Blog
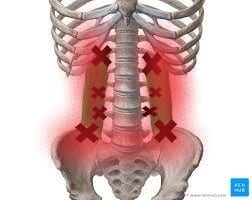
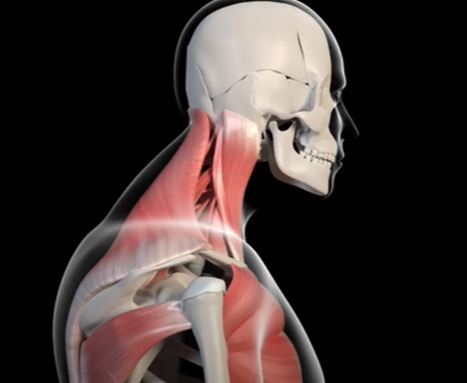
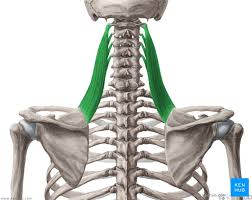
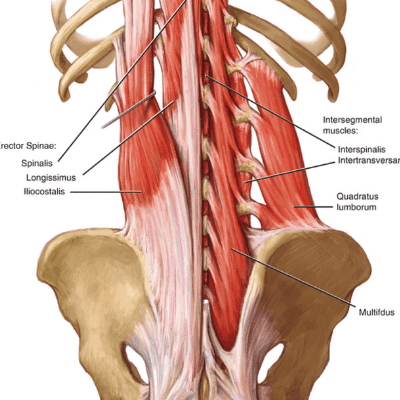
This is where my approach is different, I spend hands on time with your manipulating and releasing deep tension out of you muscles using a variety of proven
Quick Links
Useful Links
Copyright © 2014-2025 Sydney Chiropractic & Massage